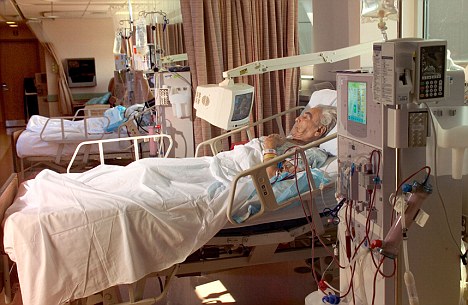
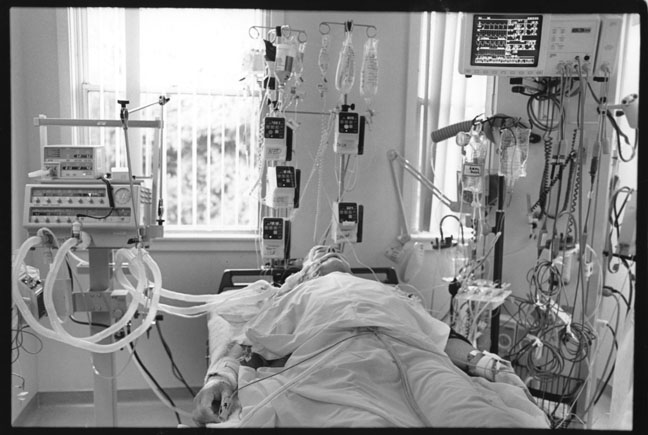
I am deeply grateful for the outpouring of compassion as well as the wealth of information I received from readers in response to my recent post, “Why Hospitals Are the Worst Place to Be When You Are Sick.” The spread of infections in hospitals has reached epidemic proportions. In this followup, I want to share some of the resources that were shared with me in emails from readers.
The Centers for Disease Control and Prevention (CDC) have identified hospital-acquired infections as the fourth leading cause of death in the United States. The CDC reported that in 2002, nearly 100,000 people died with a hospital-acquired infection (HAI), while an estimated 1.7 million people became infected. All in all, more people die per year in the U.S. with an HAI than from AIDS, breast cancer and car accidents combined.
A report published by the CDC in 2009 estimates that HAIs cost the U.S. healthcare system between $28 and $33 billion per year. Costs are such that Business Week recently identified “stopping infections in hospitals” as one of the top five methods for controlling healthcare costs.
Despite attempts to control the spread of infection, HAIs continue to wreak havoc in U.S. hospitals. The Agency for Healthcare Research and Quality (AHRQ) is the lead Federal agency charged with improving the quality, safety, efficiency and effectiveness of our healthcare. The 2009 AHRQ National Healthcare Quality Report established that hospital-acquired infections are “the most common complication of hospital care.”
In describing the scope of this problem, one reader wrote:
These infections are what’s known as antibiotic resistant pathogens or superbugs. They include Staph, MRSA, C. Diff, HIV, herpes, VRE, e. Coli, Salmonella, Norovirus, Avian Influenza A, Listeria, Acinetobacter, Rhinovirus and others. These pathogens are becoming more prevalent throughout the entire world than one could imagine. We are on the doorstep of growing a worldwide epidemic with Hospital acquired infections (HAI’s) rising at an alarming rate. A new one called NDM-1 that is believed to have originated in New Delhi was discovered mid-2010 and has now spread into many countries, killing hundreds of people. But the scary thing is that there may not be an antibiotic to kill it. So what do you do, then, when there are no successful antibiotic treatments?
New Technologies
Thankfully, the answer may be found in some of the new technologies that are being developed to combat hospital acquired infections. As one reader explained:
The World Health Organization (WHO) and the Centers for Disease Control (CDC) insist on hand sanitation at bedside in acute care facilities, each and every time healthcare workers are about to be touch the patient or his surroundings, because the hands carry infection-causing pathogens which must be inactivated to assure patient safety. The current approaches — hand washing with soap and use of alcohol rubs — have limited germicidal effectiveness, take too long (minutes for hand washing, 30 seconds for rubs) and irritate the hands due to persistent contact dermatitis, so they cannot be practically used in the WHO defined mode. Moreover, no supplier to date has come up with a means to re-sterilize gloved hands, after donning and during use, which are also vectors for transmission of dangerous germs in both the OR and the ICU. This remains an unbroken infection-causing pathway.
Here are three organizations bringing forward new technologies:
Germgard Lighting, LLC . Germgard’s technology pipeline enables a multi-tiered approach to infection prevention. Included are a UV-C technology; cost-effective bare and gloved hand sanitation process; a gas-based, room temperature medical instrument sterilization process; as well as new surface cleaning and air sterilization technologies.
IV-7 Ultimate Germ Defense. This hard surface disinfectant is currently being tested at John Hopkins Hospital. The technology is based on development of a new molecule claimed to be an effective, safe and non-toxic method of eradicating surface contaminants. The company claims that it:
- Provides 24-hour residual killing ability
- Will be awarded a Level 4 Toxicity Rating from the US EPA (no other product has received this rating in over 30 years)
- Will be validated that all the bacteria, viruses and fungi cannot become resistant to it.
Bio-Intervention Specialists . This company is dedicated to saving lives and reducing the costs associated with hospital infections. They have just received EPA registration for a new disinfecting technology that they claim is less toxic than toothpaste, environmentally friendly, yet powerful enough to kill even the toughest microbes (such as MRSA and C. diff spores) found in hospital environments. Third party efficacy and toxicity testing over the past two years has demonstrated that Electro-BioCide is entirely different from commonly used disinfectants because its kill mechanism is electrical, not chemical. As such, third party testing has demonstrated a complete kill of microbes such as MRSA and Pseudomonas in less than 30 seconds. This greatly reduces the chance for the mutation of organisms.
Patient Advocacy Resources
The Informed Patient Institute . This is an independent nonprofit organization that provides credible online information about healthcare quality and patient safety for consumers. They rate the usefulness of online health care report cards, starting with nursing homes and physicians, and provide tip sheets about what to do if you have a concern about quality in a hospital, nursing home or physician’s office.
Consumer’s Union’s Safe Patient Project. This group seeks to eliminate medical harm in our health care system through public disclosure of health care outcomes (such as hospital-acquired infection rates and incidents of medical errors) and information about health care providers (such as complaints against and license violations of physicians and hospitals). The campaign also works to improve drug safety by ensuring that consumers have full information about prescription drugs (such as in direct-to-consumer ads and access to clinical trial results), by strengthening oversight of the FDA and by ending practices that create conflicts of interest (such as drug company gifts to doctors).
The Empowered Patient Coalition. This nonprofit organization was created by patient advocates devoted to helping the public improve the quality and the safety of their healthcare, with an emphasis on high quality information and education. For example, the coalition has developed a detailed and comprehensive patient guide to hospital care which will give consumers a blue print for interacting with the health care system in ways that are safe, successful and empowering. The consumer and the patient advocate will learn how to reduce the odds of experiencing medical error and hospital-acquired infection and understand the tremendous impact they can have on patient safety and health care quality.
Books
Elizabeth L. Bewley‘s new book, “Killer Cure: Why Health Care is the Second Leading Cause of Death in America and How to Ensure That It’s Not Yours,” is focused on driving change so that health care’s purpose stops being “to deliver tests and treatments” and starts being “to enable people to lead the lives they want.” According to Publishers Weekly, this book includes useful statistics, references, a guide for further reading and excellent suggestions for patients.
Bart Windrum‘s “Notes from the Waiting Room: Managing a Loved One’s (End-of-Life) Hospitalization” offers an intelligent and heartfelt examination of what interferes with having the kind of peaceful life’s ending that most of us say we want. This is a constructive, engaging and challenging critique of the institutionalized confusion around end-of-life goals, deeply held values and biotechnology.
If you have additional resources you would like to share, please do so in the comment section of this article, so others may learn about them as well.
If you would like to know more about me and my work, please explore my website here.
Also, if you know anyone who might get value from this article please email or retweet it or share it on Facebook.